What is Bells Palsy?
Bells palsy is a situation in which there is a sudden weakness in the facial muscles. This causes one side of the face to appear wilted or hanging. This makes you laugh from only one side.
Bells palsy is also very well known as facial palsy, which can occur at any age. The exact cause of this problem is not known, but it is believed to result from swelling and redness in the nerves that control the muscles on one side of the face. It can also be a reaction after a viral infection.

Bells palsy is a temporary problem (occurring briefly) for most people. Its symptoms begin to improve within a few weeks; it takes about six months for the patient to recover completely. In a very few people, symptoms of Bells Palsy develop for a lifetime. In sporadic cases, palsy occurs again to a person.
Bells palsy Symptoms
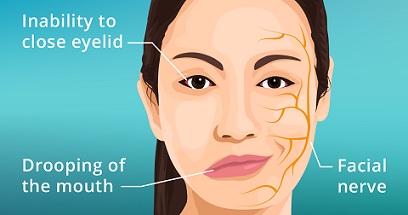
What symptoms does the bell palsy show?
Symptoms of Bells palsy may develop suddenly, which may include:
- Dripping saliva
- Feeling pain around the jaw of the affected side of the face or behind the ear
- Increased sound sensitivity in the affected side’s ear
- Headache
- Reduced ability to feel the taste
- Changes in tear and saliva (becoming more or less)
- Complete paralysis is felt by a slight weakness in the muscles on one side of the face – this can occur within a few hours to days.
- Hanging the face makes it difficult to make some facial expressions like closing the eyes or smiling.
- In some very rare cases, Bells palsy can affect the nerves on both sides of the face.
Click Here To Read: Psychology Test
When should the doctor see?
If you are experiencing any kind of paralysis or its symptoms, go to the doctor as soon as possible because you may have a stroke.
If you are experiencing problems such as weakness in the facial muscles or face hanging, then see a doctor find out the underlying cause.?
Bells Palsy Causes & Risk Factors
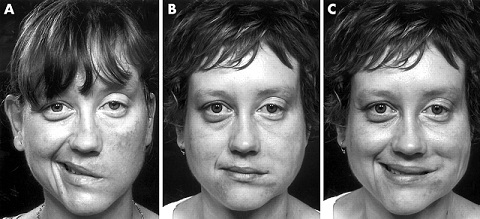
Why does bells palsy happen?
Although the exact cause of the Bells palsy is not clear, it can often be associated with viral infections. Viruses that cause Bells palsy also include some viruses that cause the following conditions:
- German measles (rubella)
- Cytomegalovirus infection
- Mumps (mumps virus)
- Flu (influenza B)
- Respiratory disease (adenovirus)
- Chickenpox and Shingles (herpes zoster)
- Hand and foot and mouth disease (Coccacivirus)
- Mononucleosis (leptin bar virus)
- Cold source and genital herpes (herpes simplex virus)
In Bells Palsy, the vein that controls the muscles of your face passes through a narrow (tight) path of bone to reach your face.?
These veins usually begin to swell due to viral infections. In addition to the facial muscles, these nerves also affect tears, saliva, the ability to taste & small bone in the mid of the ear.
When does the risk of bells palsy increase?
Bells palsy is mostly associated with the following conditions:
- Diabetes patients
- Upper respiratory tract infection such as flu or cold
- Pregnant women especially in the third trimester or for the next one week after giving birth
Apart from this, in very rare cases, some people have had to be palsy attacks more than once; someone in their family has had balsam palsy before. In these cases, the problem of Bells Palsy may be associated with genetic factors.
Click Here To Read: 50 Interesting Sleep Facts
Diagnosis of Bells Palsy
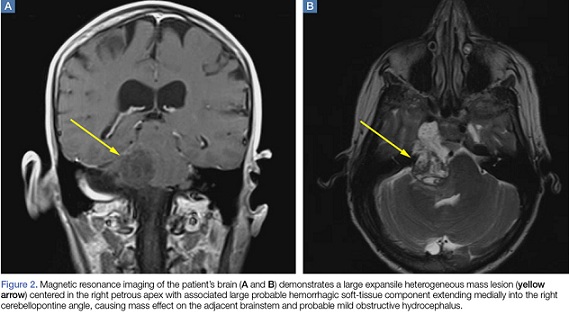
How is Bells Palsy tested?
There is no specific test available for testing facial palsy. During this test, the doctor will look at your face and ask you to move the muscles of your face like closing eyes, raising eyebrows, showing teeth and frowning.
Other conditions, such as strokes, infections, Lyme disease, and tumors, etc. can also cause weakness in the facial muscles and symptoms like bells palsy.?
If you are not clear about why you have these symptoms, then the doctor recommends the following test:
Electromyography (EMG)
This test confirms damage to the vein and determines how severely it has been damaged. The EMG test measures the nature and speed of movement of muscle activity and nerve as well as electrical impulses on the response to stimulation.
Imaging scans – Sometimes, imaging tests such as MRIs, CT scans, etc. may be required to detect other possible sources of pressure on the facial veins such as tumors and skull fractures.
Bells Palsy Treatment
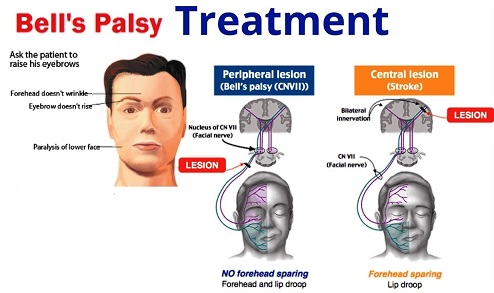
How is Bells Palsy treated?
Most people with Bells Palsy recover entirely without treatment. There is no specific treatment for belly palsy, but your doctor may suggest other medications and therapies t help you improve quickly. Very rare cases of Bells Palsy may also require surgery.
Medications:
Commonly used medicines to treat bells palsy are:
Corticosteroids
These are powerful anti-inflammatory drugs like prednisone. If these drugs reduce the swelling of the facial vein, then the protruding veins fit comfortably in the bone corridor (the place of the vein in the bone).
Corticosteroid medicines work even better if they are started within a few days of the onset of symptoms.
Antiviral drugs
The role of antiviral drugs for bells palsy is uncertain. Antiviral drugs alone showed no benefit compared to placebo (a drug, treatment, or procedure prescribed for the psychological advantage for the patient). Antivirals mixed with steroids are also unlikely to benefit.
Despite this, however, valacyclovir is given in combination with prednisone in some severe cases of balsam palsy.
Physical Therapy:
Permanent bone contraction due to paralyzed muscles can make muscles smaller. Physical therapists can teach you to properly massage and exercise the facial muscles to prevent the development of such a condition.
Click Here To Read: 10 Ways To Be A Good Mother
Surgery:
In earlier times, decompression (pressure reduction procedure) surgery was used. This surgery procedure used to open the hole in the bone through which the facial veins pass.
Nowadays, decompression surgery is not suggested, as this surgical procedure is associated with permanent facial nerve damage and hearing loss.
In rare cases, plastic surgery is required to fix facial nerve problems permanently.
Bells Palsy Complications

What problems can cause palsy?
Cases of the moderate condition of Bells palsy begin to disappear within a few months, but the more severe cases involving complete paralysis may have a different recovery (recovery period) process. Complications resulting from this may include:
- Damage to the facial veins that cannot be recovered.
- Partial or complete blindness may develop due to dryness and scratching in the cornea in the eye of the affected area, which is not closed.
Fibers regrow, resulting in other nerves functioning automatically when you try to use some veins. This condition is also called Synkinesis; for example, when you smile, the eye on the affected part automatically closes.
Note: Depression Cure does not provide any type of medical advice, diagnosis, or treatment.
Post | Title | Ratings | Link |
22 Ways To Deal With Depression | |||
45 Ways to Get Rid of Depression | |||
20 Simple Ways to Overcome Depression | |||
25 Ways To Make Yourself Emotionally Numb |





